What is atopic eczema in children?
Atopic eczema, also known as constitutional eczema, is a long-term inflammatory skin condition characterized by intense itching, redness, and dryness. The disorder can start at any age, but it mainly occurs in young children. Often, the first signs appear as early as the first months of life, usually between three and six months of age.
The word “atopic” refers to an inherited predisposition to develop hypersensitivity disorders. Children with atopic eczema often have other atopic conditions in the family, such as asthma, hay fever, or food allergies. These disorders often occur together in the same person or within one family.
With atopic eczema, your child's skin barrier does not work optimally. Healthy skin forms a protective layer that retains moisture and keeps harmful substances out. In children with eczema, this barrier is weakened, so that the skin dries out more quickly and is more sensitive to stimuli. This explains why your child's skin reacts so strongly to things that other children don't notice. It's important to know that atopic eczema has nothing to do with poor care or hygiene, but is caused by your child's genetic predisposition.
Heb je last van Atopic Eczema in Children?
Laat je huid beoordelen door een erkende dermatoloog via de Skindr app. Upload foto's en krijg binnen 48 uur een diagnose met persoonlijk advies. Geen wachtkamer, geen verwijsbrief nodig.
How does atopic eczema occur in children?
The exact cause of atopic eczema is not yet fully understood, but several factors come together to develop and worsen the condition.
The most important factor is heredity. If one or both parents have or had atopic eczema, asthma, or hay fever, your child is much more likely to develop eczema as well. The risk is highest among children whose both parents have an atopic disorder.
In children with eczema, the skin does not produce enough lipids (fats) and moisture-binding substances. As a result, the outer layer cannot perform its protective function properly. Moisture evaporates faster, the skin dries out and allergens can penetrate more easily. Your child's immune system overreacts to these stimuli, leading to inflammatory reactions that cause the typical red, swollen, and itchy patches.
Atopic eczema progresses in flares, alternating periods of serious symptoms with quieter periods. Various factors can trigger such an upsurge. Skin irritation is a common trigger: sweating, scratching, rough clothing (especially wool), and frequent soap washing can make symptoms worse.
Stress and emotions also play a role, even among young children. Tension, anxiety, or major changes can cause or worsen an upsurge. It is often a vicious cycle: eczema causes stress and discomfort, and that stress makes the eczema worse. Contact allergies play a role in some children, i.e. reactions to substances that are applied to the skin. To a lesser extent, diet plays a role, but not every child with eczema also has food allergies.
Climate and seasons also influence eczema. Many children suffer more in the winter, when the air is drier due to heating. Summer has mixed effects: sunlight can be healing, but sweating and air conditioning actually make things worse.
Symptoms and characteristics of atopic eczema in children
The most important and bothersome symptom of atopic eczema in children is intense itching. This itch can be so intense that it disrupts your child's sleep and affects his or her behavior. Small children can become irritable and crying due to the constant itching.
The rash may look different depending on your child's age and the phase of the eczema. You can often see red spots on dry, scaly skin. The skin can feel rough and thickened, especially in areas where eczema has been around for a long time. Sometimes you'll see small blisters or bumps where fluid can come out, called wet eczema. This moisture dries up and forms scabs.
Continuous scratching causes scratch wounds that can become infected with bacteria. You can recognize this by suppuration and yellowish crusts. It is important to treat these infections quickly to prevent further complications.
In children with lighter skin, the eczema is often bright red. In dark-skinned children, it may look purple, dark brown, or gray. Dark or lighter spots after healing usually fade over time. The eczema looks different in each child.
The constant itching, insomnia and visible skin problems can take a heavy toll on both your child and the whole family. Kids can be ashamed of their looks, especially as they get older. Sleep deprivation due to nocturnal itching affects behavior, school concentration, and mood. As a parent, caring for a child with eczema can make you tired and stressed.
Where does atopic eczema occur in children?
Atopic eczema appears in specific areas of the body, depending on your child's age.
In babies and very young children, eczema mainly occurs on the face, particularly on the cheeks, forehead, and chin. The scalp may also be affected, as well as the outside of the arms and legs. The diaper zone is usually spared, which helps distinguish eczema from other skin conditions.
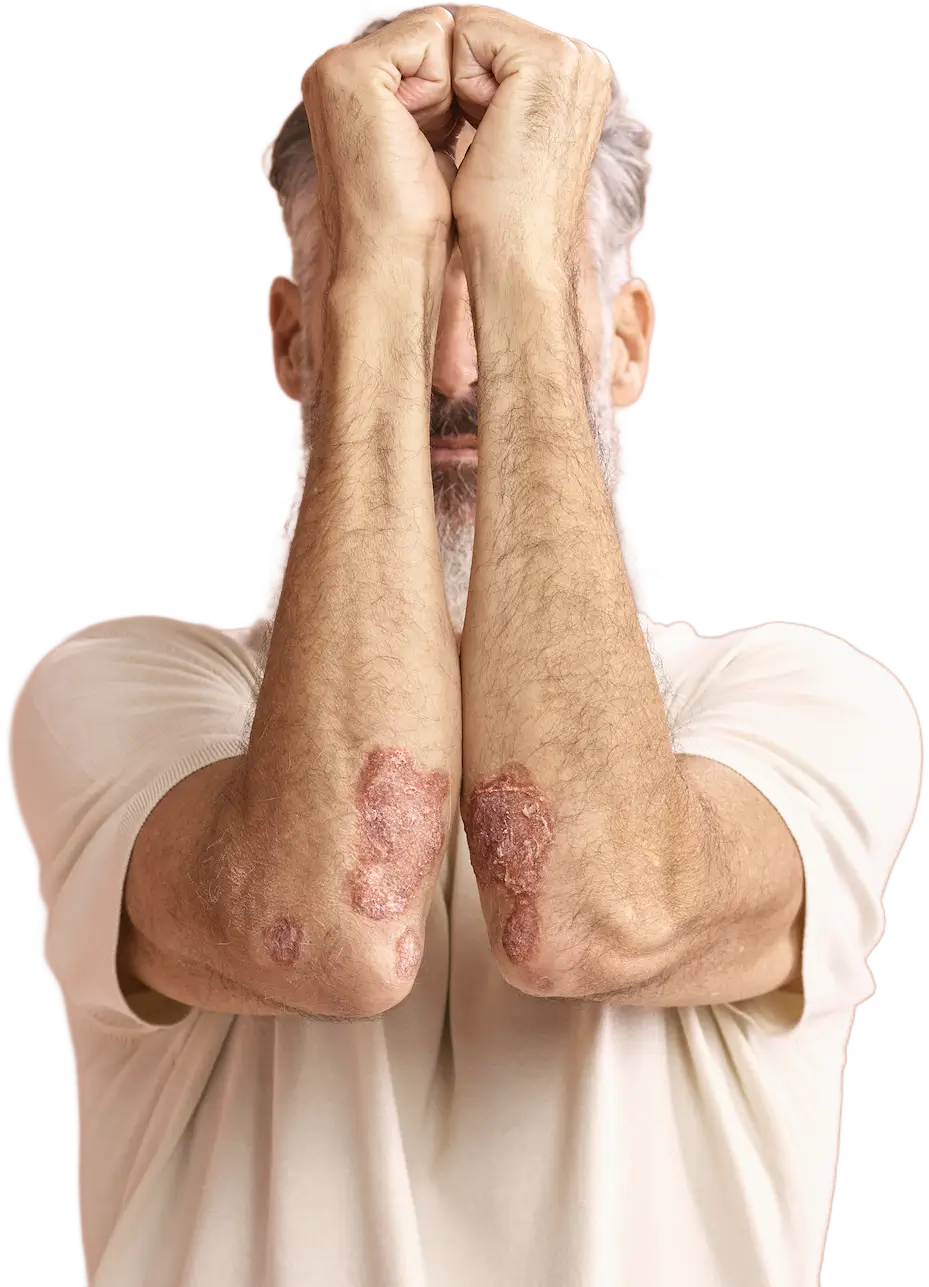
As children get older, the location changes. In toddlers and older children, it mainly occurs in the skin folds: the inside of the elbows, the knee cavities, the wrists and ankles. The neck is also often affected, as are the hands and feet. In severe cases, eczema can occur over large parts of the body. The rash is often symmetrical, which means that the same areas are affected on both sides of the body.
Heb je last van Atopic Eczema in Children?
Laat je huid beoordelen door een erkende dermatoloog via de Skindr app. Upload foto's en krijg binnen 48 uur een diagnose met persoonlijk advies. Geen wachtkamer, geen verwijsbrief nodig.
Treatment of atopic eczema in children?
The most important thing to know is that atopic eczema is a chronic condition that cannot be completely cured. The treatment therefore focuses on taking good care of the skin to restore its barrier function, and treating flare-ups to relieve symptoms.
The basis of each treatment is to moisturize the skin daily, even when there is no active eczema. Hydrating creams, ointments, lotions, and bath oils help keep skin moist and strengthen the skin barrier. You can use these products multiple times a day if the skin benefits.
The best time to hydrate is right after bathing, when the skin is still moist. Gently pat the skin dry and then apply the hydrating product immediately. Ointment is often more effective than cream for very dry skin because ointment contains more fat and evaporates less quickly. Preferably choose hypoallergenic products without perfume and colorants, as these substances can irritate sensitive skin extra. An expensive product isn't necessarily better than a simple base cream. For young children and their parents, there are sometimes special “smear schools” available where you can learn how to best care for the skin. Ask your doctor or healthcare provider about options in your region.
When your child has a stroke, the doctor usually prescribes cortisone creams or ointments. Cortisone is a powerful anti-inflammatory that helps reduce redness, swelling, and itching. There are different strengths, and the doctor will choose the right strength depending on your child's age, the severity of the eczema and the location on the body. For young children, the doctor chooses milder cortisone than in older children. Facial skin always gets a milder treatment than the skin on the arms or legs.
It is important to use cortisone products exactly as prescribed by the doctor. Some children occasionally need to take a low dose preventively to prevent new flare-ups. Modern children's cortisone creams are safe when used correctly. The benefits of treating eczema far outweigh the small risks of proper use.
If the eczema does not respond well to the standard treatment, the doctor may refer you to a dermatologist. This specialist may prescribe other anti-inflammatory creams or ointments that are not made from cortisone. These are recommended as a follow-up treatment or to alternate with cortisone ointment. However, because these ointments are still less powerful and cause a burning sensation on active eczema skin, they cannot fully replace the use of cortisone yet.
In very severe cases, light therapy (phototherapy) may be an option, although it is less common among young children. In very severe forms, treatments in pill or injection form are also available, but this is only done under intensive supervision in specialized centers for children. Dietary supplements are sometimes recommended, but scientific research shows that they usually provide no significant improvement.
The duration of treatment varies greatly from child to child. Some children have sufficient control over their symptoms with good skin care and occasional cortisone cream. Others require more intensive, long-term treatment. The good news is that many children's eczema improves as they get older. For most children, the symptoms subside after puberty, although around half can still have some form of eczema in adulthood.
What does not work against atopic eczema in children
There are many misconceptions and myths about atopic eczema. It's important to know what isn't effective so you don't waste time and money on useless treatments.
Although many children suffer less as they get older, that doesn't mean you don't have to do anything. Without good skin care and treatment, eczema will not improve and may even worsen, with a greater risk of infections and scarring. Active care is essential.
A common misunderstanding is that a special diet or avoiding certain foods will cure eczema. For most children, nutrition does not play a role. Only a proven food allergy (determined by an allergy test) can avoiding that specific food help, but this only occurs in a small group. Strict diets without a medical indication can be harmful to your child's growth and development. Never rule out important food groups without medical advice.
While hygiene is important, bathing or showering too often can actually make eczema worse. Daily bathing with warm water and plenty of soap dehydrates the skin and further weakens the skin barrier. Limit bathing to two to three times a week with lukewarm water, use as little soap as possible, and add bath oil. Always moisturize the skin immediately after bathing.
Many alternative treatments are being touted for pediatric eczema, from special creams to homeopathy and nutritional supplements. Most of them have no scientific proof of effectiveness. Some may even be harmful or cause allergic reactions to your child's sensitive skin. Always talk to your doctor before trying new treatments.
While rough clothing and certain detergents can irritate eczema, they are rarely the main cause. Replacing all your detergents and clothes usually won't solve the problem. However, it is wise to avoid raw wool and synthetic fabrics and choose soft, breathable cotton clothing. Wash new clothing before wearing to remove excess chemicals.
Frequently asked questions about atopic eczema in children
Is Atopic Eczema Contagious?
No, atopic eczema is definitely not contagious. Your child cannot transmit it to other children by touching, sharing toys, or other forms of contact. It is a disorder that results from your child's genetic predisposition and how his or her skin and immune system function. Even when eczema becomes infected with bacteria, the underlying condition remains non-transmissible.
Will this always bother my child?
Most children with atopic eczema experience improvement as they get older. For many children, the symptoms decrease during puberty. Around half of the children with eczema have little or no problems as adults. The other half can have complaints to a lesser or greater extent. It is difficult to predict how your child will fare, but with good care and treatment, the symptoms can usually be well controlled.
Can my child do normal activities such as swimming and exercising?
Yes, your child can basically do all normal activities. Swimming can even be good, but rinse your child thoroughly after swimming in chlorinated water and then apply a moisturizer immediately. When exercising, it is important to shower and hydrate quickly afterwards, as sweat can irritate the eczema. Don't let eczema limit your child's social activities, this is important for his or her development.
When should I see a doctor?
See a doctor if you see symptoms of eczema in your child for the first time and are not sure what it is. Also visit the doctor if the familiar eczema suddenly gets worse, does not respond to the usual treatment, shows signs of infection such as suppuration or yellow scabs, or if the itching is so severe that it seriously affects your child's sleep and behavior. If the eczema affects your child emotionally or if you are overwhelmed as a parent, it is also important to discuss this with the doctor.
Does getting rid of a pet help?
This is a tough question that many families struggle with. Only if there is a proven allergy to the specific pet (determined by allergy tests) and if the eczema clearly worsens due to contact with the animal, giving the pet away can be considered. For most children with eczema, however, this is not necessary. Always discuss this thoroughly with the doctor before making such a drastic decision, as giving away a beloved pet can be emotionally difficult for your child.
What can I do about my child's itching?
Itching is often the most difficult aspect of eczema, especially in young children who don't understand why they shouldn't scratch. Keep your child's nails cut short to limit damage caused by scratching. For babies, you can use thin cotton mittens while sleeping. Make sure the bedroom is cool, as heat worsens the itching. Distraction can also help: try to keep your child busy with activities that distract attention from the itching. The doctor may also prescribe antipruritic medication if the itching is extreme.

.webp)







.avif)

-min.avif)

-min.avif)





.svg)
