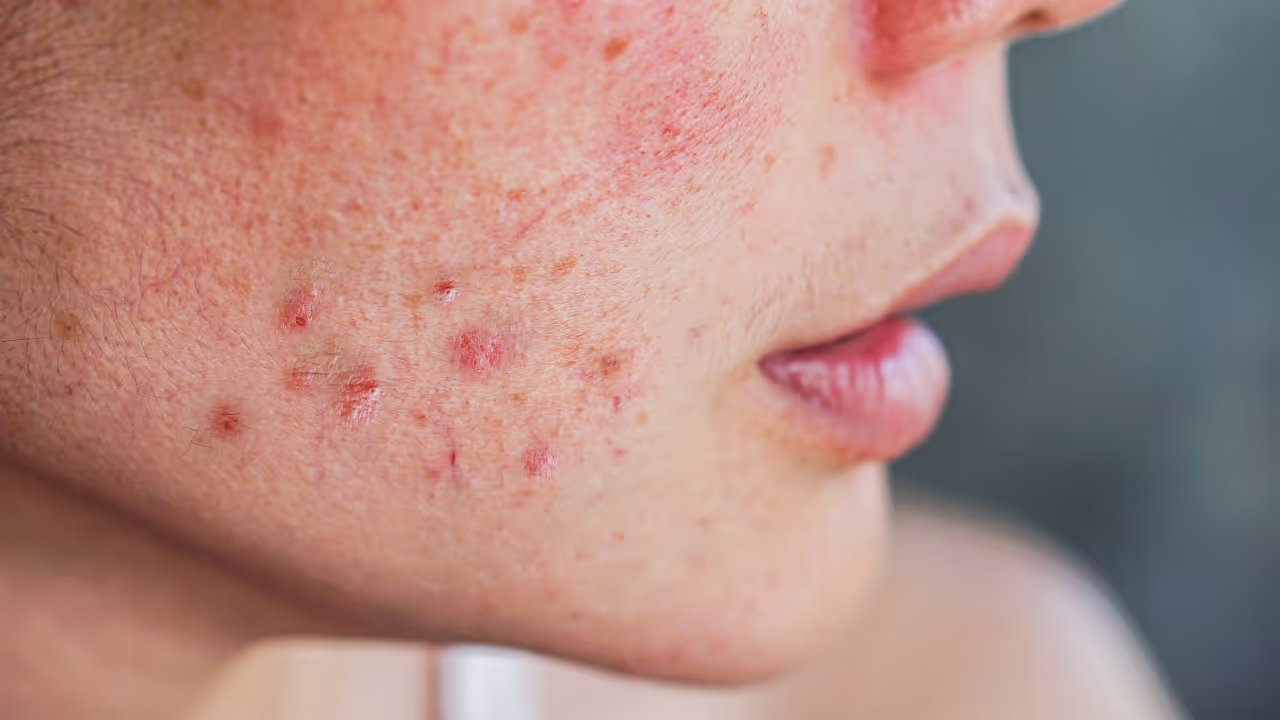
What is a facial rash?
Facial rash is a generic name for different types of skin changes that can occur on your cheeks, forehead, chin, nose, or around your eyes and mouth. These are abnormalities in the normal skin structure and color that can take various forms.
Often, the rash looks red and inflamed. Redness occurs because blood vessels in the skin are dilated due to inflammatory reactions. This redness may be uniform or occur in patches. Itching is a frequent symptom that causes a lot of discomfort. The urge to scratch is great, but this usually worsens the situation.
Peeling often occurs with facial rashes. The skin peels or flakes come off, which is associated with an accelerated renewal of skin cells. This can give the skin a dry, rough appearance. Bumps or pimples may be part of the rash. These minor imperfections may be filled with fluid, pus, or simply be solid tissue.
The location of the rash on the face sometimes provides clues to the cause. Rash around the mouth may indicate perioral dermatitis. Red spots on the cheeks and bridge of the nose are reminiscent of lupus or rosacea. Rashes along the hairline or in the eyebrows may be seborrheic eczema.
Because there can be so many different causes, it is sometimes difficult to determine for yourself what is going on. The duration, course and accompanying symptoms help make the correct diagnosis.
Do you suffer from Facial rash?
Have your skin assessed by a licensed dermatologist via the Skindr app. Upload photos and get a diagnosis with personal advice within 48 hours. No waiting room, no referral required.
How does a facial rash occur?
Facial rashes can occur due to irritation, an underlying skin condition, or an infection.
Irritation is common and usually temporary. Cosmetics, hair removal, shaving, or drying soaps can cause red, irritated, or scaly skin.
Various skin disorders manifest themselves on the face. Acne occurs due to clogged pores, excessive sebum production, and the presence of Cutibacterium acnes, often made worse by hormones. Rosacea is a chronic condition with overreactive blood vessels, resulting in persistent redness and inflammation. Eczema develops as a reaction to allergens or from a hereditary predisposition.
Specific triggers can trigger or worsen disorders: sunlight (for lupus and rosacea), stress (acne and eczema), and hormone fluctuations (can cause melasma).
Infections occur when bacteria, viruses, or fungi invade the skin. Impetigo is caused by bacteria, often after skin damage. Ringworm is a fungal infection, often transmitted via infected animals. Herpes simplex virus causes cold sores around the lips.
A weakened immune system makes infections easier and can make existing conditions worse. Autoimmune diseases such as lupus are also caused by a dysregulated immune system.
Genetic factors and skin type determine your sensitivity. If family members have certain conditions, you are at increased risk. Light skin types are more sensitive to sun damage and rosacea, darker skin types to pigmentation problems.
Symptoms and characteristics of a facial rash
The symptoms of facial rash vary greatly depending on the underlying cause. Recognition of specific characteristics helps identify the disorder.
Acne is a combination of different types of impurities. Comedones or blackheads are clogged pores that can be white, yellow, or black. Papules are small red bumps with no visible pus that can be painful when touched. Pustules are pimples filled with yellow or white pus that look inflamed. In severe cases, deep, painful lumps under the skin can develop that last for a long time.
Rosacea appears as sudden redness that lasts longer than blushing. The redness may come and go but gradually becomes more persistent. Tiny blood vessels become visible as fine red lines, especially when you look in the mirror up close. There may be bumps and pimples that look like acne but without the typical blackheads. In some people, the skin gradually thickens, which can give a lumpy appearance. The skin often feels hot and may be burning.
Facial eczema is characterized by dry, red patches that are itchy and slightly scaly. The skin may appear cracked and feels rough when touched. Scratching can cause open areas where clear moisture comes out of the skin. The itching is often worse at night or when it's warm. The skin can look duller and the loss of its natural glow is noticeable.
Seborrheic eczema appears as red patches covered with greasy, yellow flakes that feel different from the dry flakes in common eczema. The flakes can be sticky and are difficult to remove completely. It is often itchy and the flakes can be difficult because they are conspicuous, especially in the eyebrows or around the wings of the nose. The skin underneath is red and may appear slightly swollen.
Perioral dermatitis causes small red pimples that may look like acne or eczema but have a different pattern. The skin feels burning and can peel, causing a dry, tense feeling. A narrow strip of normal skin directly around the lip edge is characteristic, which helps to distinguish this condition from other types of rash. The condition can last for weeks to months without treatment.
Lupus erythematosus shows the characteristic butterfly-shaped red rash that is remarkably symmetrical. The skin may peel and feel warm when touched. The rash worsens markedly after exposure to sunlight, even after brief exposure. There may also be round, disc-shaped lesions that feel thicker and can leave permanent discoloration.
In impetigo, you first see red spots that quickly grow into blisters filled with cloudy fluid or pus. These blisters burst open easily and leave behind typical golden yellow scabs that look sticky. It itches and is highly contagious, so it can spread quickly to other facial areas or to other people. The skin around the scabs is often red and inflamed.
Herpes cold sores start with a burning, stinging sensation that precedes the visible blisters a few hours to a day. After that, clusters of small blisters filled with clear fluid appear that are close together. The blisters feel tense and can be painful. They dry out into scabs that fall off after about a week. It recurs regularly in the same place, often triggered by stress, illness or sunlight.
Ringworm appears as round or oval red spots with a distinctive raised edge and a paler center, which creates a ring-shaped pattern. The edge may be slightly scaly and sometimes small sores are visible. It usually itches and can spread in concentric circles if left untreated. The edges are often sharply defined.
Where does a facial rash appear?
The T-zone (forehead, nose, chin) is a common location for acne and seborrheic eczema due to increased sebum production. The forehead can be full of bumps, the nose often has blackheads, and red spots with greasy flakes appear along the hairline.
The cheeks are vulnerable to various types of rashes. Rosacea typically appears here with persistent redness and visible blood vessels. The butterfly-shaped rash in lupus extends across both cheeks and the bridge of the nose. Eczema in children often occurs on cheeks with red, scaly patches.
Around the mouth, perioral dermatitis is typical, with small red pimples and often a free zone directly against the lip edge. Impetigo also often starts here with golden yellow scabs. Cold sores appear on or around the lips.
The eyebrows and hairline are typical of seborrheic eczema, with red patches and greasy, yellow flakes.
The folds around the nose and mouth (nasolabial folds) are susceptible to seborrheic eczema because they collect sebum and fluid.
The area around the eyes is vulnerable to allergic contact eczema, often caused by eye makeup. The skin here is thinner and more sensitive.
The chin and jawline are typical of hormonal acne in women, with deep pustules linked to the menstrual cycle. In men, shaving can cause folliculitis here.
Some disorders are not confined to the face. Rashes on other body parts may help with diagnosis.
Do you suffer from Facial rash?
Have your skin assessed by a licensed dermatologist via the Skindr app. Upload photos and get a diagnosis with personal advice within 48 hours. No waiting room, no referral required.
Treatment of a facial rash
The treatment for facial rashes is customized and depends very much on the underlying cause. A good diagnosis is essential for effective treatment.
In case of irritation from cosmetics or skin care products, the first advice is to stop all suspicious products. Instead, use gentle, fragrance-free products designed specifically for sensitive facial skin. It can take a few weeks for the skin to recover. A hypoallergenic moisturizer helps restore the skin barrier and prevents further dehydration.
Acne is treated based on severity. Mild acne, mainly blackheads, responds well to topical treatment with specific active substances that help keep pores open and have a mild antibacterial effect. In the case of inflammatory acne (acne with a lot of redness and subcutaneous nodules), the topical remedy helps to calm the inflammatory response in the skin. This way, the pimples can heal better and new inflammations are limited. We do not use this cream primarily to kill bacteria, but mainly because it has an anti-inflammatory effect.
Moderate to severe acne often requires oral medication for several months. In women, certain birth control pills can help by regulating hormonal influences. In persistent cases, a dermatologist may prescribe a powerful remedy that drastically reduces sebum production, but this requires intensive guidance due to possible side effects such as dry skin, lips and sometimes mood swings.
Rosacea is not curable but easy to manage. Topical anti-inflammatory creams are the first-line treatment and reduce the inflammatory response in the skin. In more severe rosacea, oral medications can help deal with inflammation from within. Avoiding triggers such as spicy food, alcohol, extreme temperatures and stress is crucial for long-term success.
Eczema the face requires careful treatment because the facial skin is thin and sensitive. A mild anti-inflammatory cream can be used for flare-ups, but only briefly and under the guidance of a doctor. For long-term use, alternatives exist that are safer for facial skin. Consistent use of moisturizer to support the skin barrier is essential.
Seborrheic eczema responds well to antifungal treatments, as a yeast plays a role in this condition. These are available as face creams. Here, too, mild anti-inflammatory creams can help with pronounced inflammations, but again only for short periods. For the scalp, special shampoos are available that also help with facial symptoms, especially along the hairline.
Perioral dermatitis requires the discontinuation of all creams and cosmetics, especially anti-inflammatory preparations or cortisone in other forms, such as puffers and nasal sprays if used. The skin takes time to recover, which can take several weeks. The doctor may prescribe topical or oral treatment that reduces the inflammatory response. It's important to be patient as the condition can temporarily worsen before improvement, which can be frustrating.
Infections such as impetigo are treated with antibiotic ointment or, in the case of extensive infections, oral antibiotics. Good hygiene is essential to prevent the spread. Use separate towels, wash your hands often, and don't touch your face. Herpes cold sores can be treated with antiviral cream or tablets, especially if they recur frequently or are severe. For best results, start the treatment at the first stimulation.
Fungal infections such as ringworm require antifungal medicines, first as a cream and, in persistent cases, as tablets. The treatment should continue long enough, usually a few weeks, even if the rash appears to have disappeared. This prevents relapse because the fungus can sit deeper in the skin than is visible.
More complex disorders such as lupus require treatment by a specialist. This may include anti-inflammatory creams, specific oral medications that regulate the immune system, or other treatments depending on the severity and whether other organs besides the skin are involved.
In all cases, sun protection is important. Use a sunscreen with at least SPF 30 daily, even on cloudy days and in the winter. UV radiation can worsen many skin conditions and trigger inflammation. Opt for mineral
What doesn't work against a facial rash?
There are many misconceptions about treating facial rashes that are not only ineffective, but sometimes even worsen the situation.
The idea that you can squeeze out acne to get rid of pimples faster is counterproductive. Squeezing pushes bacteria deeper into the skin, which worsens inflammation and can lead to larger, more painful pustules. It can cause permanent scarring, especially on the face where the skin is thinner and scar tissue remains more conspicuous. Leave pimples alone or have them professionally treated by a dermatologist.
Washing the face too intensively in the hope of washing away the rash actually dries out the skin. This stimulates sebum production as compensation, which can make acne worse. Even with eczema and rosacea, frequent washing with soap makes the skin drier and more vulnerable to inflammation. Wash your face up to twice a day with a mild, pH-neutral cleanser and then gently pat dry instead of rubbing.
Self-medication with strong anti-inflammatory creams that you still have at home or buy over the internet is risky. These creams can provide short-term improvement, but make facial skin thinner and more vulnerable when used for a long time. They can also make rosacea worse or cause perioral dermatitis, which can make you feel better. Use these creams only under medical supervision.
Applying alternative or natural remedies such as essential oils, lemon juice, or toothpaste to acne or other rashes may cause irritation and allergic reactions. What is natural is not automatically safe for your skin. Lemon juice, for example, makes the skin extremely sensitive to sunlight and can cause burns. Essential oils are concentrated substances that can cause skin irritation. Stick to medically proven treatments.
The idea that sunbathing improves acne or other rashes is wrong. UV radiation initially seems to improve because it dries the skin and masks inflammation caused by tanning the skin, but this is short-lived. This is often followed by a rebound effect with more pimples than before. In addition, UV radiation accelerates skin aging and increases the risk of skin cancer and can cause less effective healing. In conditions such as lupus and rosacea, sunlight actually worsens the rash dramatically.
Experimenting with all possible creams and lotions at the same time makes it difficult to determine what works and what doesn't. It also makes your skin more vulnerable through the combination of different active ingredients. In the event of a problem, do not consider that the treatment itself may be the cause. Introduce new products one by one and give each product a few weeks to take effect before giving up.
Ignoring a rash in the hope that it will go away on its own rarely works. Some conditions such as acne and rosacea are chronic and require continuous treatment to stay under control. Early treatment prevents scarring and long-term inflammations that are more difficult to treat. Infections also deserve rapid attention to prevent the spread and complications such as deep skin infections.
Frequently asked questions about facial rash
Is facial rash contagious?
This depends on the cause. Infections such as impetigo, cold sores, and yeast infections are contagious and can be transmitted through direct contact or shared use of towels, washcloths, and pillows. Skin conditions such as acne, eczema, rosacea, and psoriasis are not contagious. You can't contract them through contact with someone who has these conditions. However, they can be hereditary, so they are more common in families.
How long do facial rashes last?
The duration varies greatly by condition. Acute rash due to irritation often disappears within a few days to weeks after stopping the irritant. Acne is a chronic condition that can last for months to years, especially during puberty. Rosacea and eczema are also chronic with periods of flare-ups and rest. Infections such as impetigo heal with treatment within a week to ten days. It is important to continue treatment even if the rash appears to be improving.
Can I use makeup for facial rashes?
You can use makeup for acne and rosacea, but choose products that are specially developed for sensitive or acne-prone skin and that do not clog pores. Mineral makeup is often a good choice because it contains fewer irritating ingredients. In case of active eczema or infections, it is better to avoid makeup until the rash has healed. Makeup can aggravate irritation and trap bacteria against the skin. Always cleanse your face thoroughly before going to bed.
When should I see a doctor?
Consult a doctor if the rash does not improve after two weeks of self-treatment, if the rash is painful or accompanied by a fever, if the rash is extensive or severe, or if you feel uncertain about the cause. Even if you have a lot of itching that does not respond to over-the-counter medicines, or if the results affect your social life, professional help is useful. In the case of scabbing infections or weeping wounds, medical treatment is necessary to prevent the spread.
Does a diet change help against facial rashes?
The link between diet and skin conditions is complex and does not work the same for everyone. A diet lower in dairy and sugar may help with acne, although the effects vary from person to person. In rosacea, certain foods such as spicy foods, alcohol, and hot drinks can trigger flare-ups. Eliminating these triggers can help. For eczema, food allergies are sometimes a factor, especially in children. An elimination diet under the guidance of a dietician can then be useful. Extreme diets without medical supervision are not recommended.
Do scars come from facial rashes?
Acne can leave scars, especially in severe inflamed forms or when pimples are pinched. Early and adequate treatment helps prevent scarring by quickly controlling inflammation. Impetigo and herpes don't usually leave scars if they're treated properly and don't scratch you. Deep infections or serious inflammations can cause scarring. Lupus often leaves permanent scars in areas where injuries have occurred. Good treatment and avoiding scratching are crucial to limit scarring.

.webp)