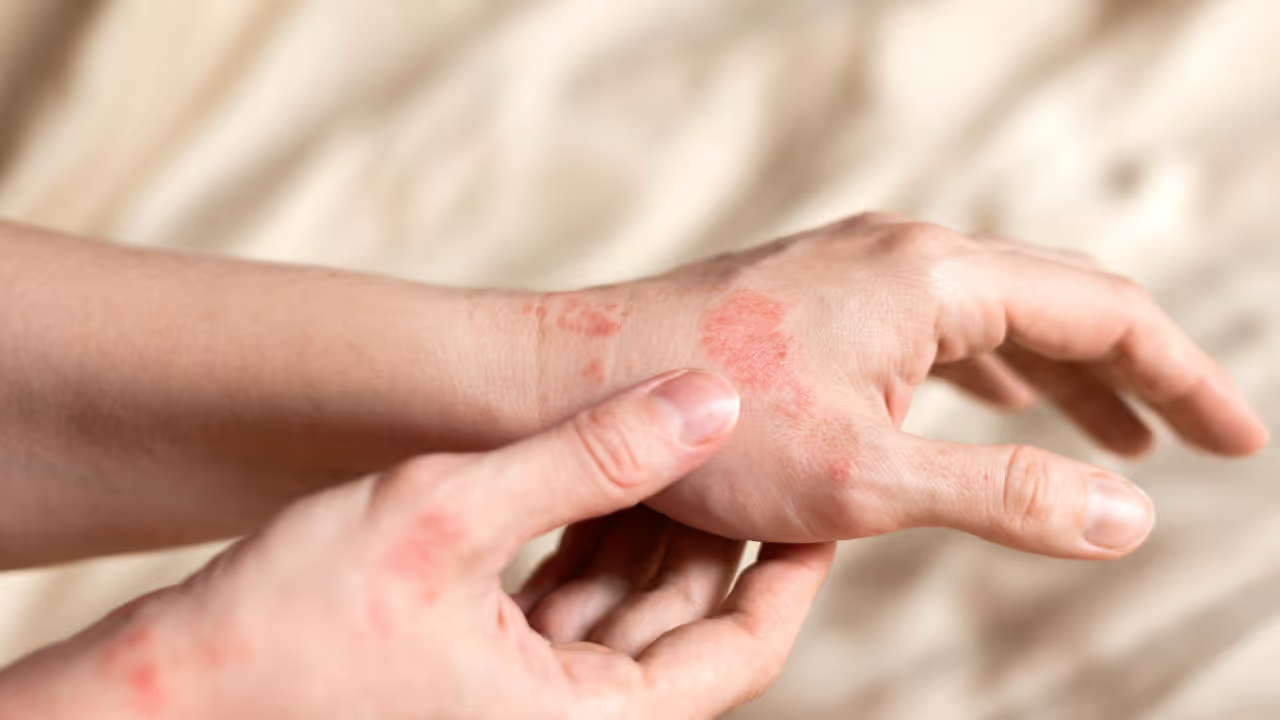
What is hand eczema?
Dermatitis literally means inflammation of the skin. It is a collective name for various skin conditions where the skin becomes inflamed. In hand dermatitis, this inflammation is specifically localized to the hands, although sometimes the wrists may also be affected. The inflammation can occur acutely, i.e. sudden and severe, or be chronic and last for months.
There are various causes that can cause hand dermatitis. The two most common forms are allergic contact dermatitis and toxic contact dermatitis. In allergic contact dermatitis, your immune system has become hypersensitive to a certain substance. After repeated contact with that substance, your skin reacts with an inflammatory response. This can happen after weeks, months, or even years of trouble-free contact with a product.
Toxic contact dermatitis, also known as irritant contact eczema, occurs due to direct damage to the skin by irritants. These can be strong chemicals such as bleach or solvents, but seemingly harmless substances such as water and soap can also damage the skin when contacted repeatedly. In contrast to allergic reactions, toxic dermatitis does not require you to become sensitive first, the damage occurs immediately.
Nummular eczema is a form of coin-shaped, sharply delimited areas that are often very itchy. The cause of this is not entirely clear. Atopic dermatitis, also known as constitutional eczema, is an inherited disorder where the skin is naturally drier and becomes inflamed more quickly. People with atopic dermatitis often also have other allergic conditions such as hay fever or asthma.
Fungal infections, especially ringworm, can also affect the hands and cause symptoms similar to dermatitis. More rare are conditions such as scabies, psoriasis, or lichen planus that can cause injuries to the hands.
Certain factors increase the risk of developing hand eczema. Smoking and excessive alcohol consumption appear to be risk factors. Working in humid conditions, such as in the hospitality industry, healthcare or cleaning, increases the risk significantly. Work in the food industry where you have to wash your hands regularly and come into contact with various ingredients is also a risk factor. Sweating, dirt and skin chafing contribute to the development of hand eczema.
An interesting finding is that children who have hand dermatitis at an early age have a high chance of getting it as adults as well. This suggests that there is a predisposition that remains present for life.
Do you suffer from Hand eczema?
Have your skin assessed by a licensed dermatologist via the Skindr app. Upload photos and get a diagnosis with personal advice within 48 hours. No waiting room, no referral required.
How does hand eczema occur?
The development of hand eczema is often a gradual process that starts with minor changes in the skin. In toxic contact dermatitis, repeated exposure to irritants plays the leading role. Water is one of the main culprits, although this sounds surprising. Repeated wetting and drying of the hands causes the natural fats from the skin to be lost. The skin barrier is damaged and the skin can no longer retain moisture properly.
Soap enhances this effect. Soap dissolves not only dirt, but also the protective fat layer of the skin. For people who wash their hands dozens of times a day, such as in the healthcare or food industry, the skin has no chance to recover. The damaged skin barrier now also lets other irritants through more easily, triggering a vicious cycle.
Detergents, solvents, degreasing agents and other chemicals accelerate damage. Mechanical stress such as rubbing and sanding also contributes. Think of working with paper, cardboard, or wearing work gloves that rub against the skin.
In allergic contact dermatitis, the process is different. Here, you first have to become sensitive to a certain substance, a process called sensitization. This can happen after a few weeks of exposure, but sometimes only after years of trouble-free contact. Once sensitized, any new exposure to that substance will trigger an inflammatory response. The immune system recognizes the substance as foreign and reacts excessively.
Common hand allergens include nickel in jewelry and tools, rubber chemicals in gloves, perfumes and preservatives in soaps and creams, and epoxy resin for construction workers. Plant substances such as primrose or tulip bulbs can also cause contact allergies among gardeners.
A special aspect of hand eczema is the role of fungal infections on the feet. A fungal infection between the toes or the sole of the foot can trigger a reaction on the hands without the fungus itself being there. This is called an id reaction and is an immunological phenomenon. Treatment of the foot fungus therefore makes the hand problems disappear.
Atopic dermatitis on the hands is often part of a wider picture that also affects other parts of the body. The predisposition to sensitive, dry skin means that people with atopic eczema are extra sensitive to both irritants and allergenic substances. Their hands therefore react more quickly and more strongly to the same stimuli that do not cause problems for others.
Stress and mental factors can make dermatitis worse. Stress lowers immune function and can make itching worse, leading to more scratching. Scratching further damages the skin and maintains inflammation.
Symptoms and characteristics of hand eczema
The most characteristic symptom of hand eczema is itching. This itching can range from mildly irritating to unbearable and may worsen at night. The tendency to scratch is high, but scratching further damages the skin and worsens inflammation. Some people unconsciously scratch at night, which makes the situation even worse.
The skin is red, which can range from a slight pink color to a bright red color in case of acute inflammation. This redness is due to widening of the blood vessels in the skin in response to the inflammation. In dark-skinned people, the redness is less visible, but the skin may be darker or lighter in the affected areas.
Peeling is another typical feature. The skin sheds dead skin cells faster than normal, which is expressed in flakes. These can be fine as a type of powder, or larger flakes. Very dry skin can cause deep cracks, especially in areas that move a lot, such as the knuckles. These cracks can be painful and bleed.
In acute dermatitis, small blisters may form. These blisters are filled with clear fluid and may itch or burn. When they open, fluid leaks out, which is called wet eczema. This wet stage is often the most uncomfortable. The skin feels raw and sore. The moisture can further irritate the surrounding skin.
In chronic dermatitis, the skin is actually thickened and hardened. This process is called lichenification and is the result of prolonged scratching and rubbing. The skin lines deepen and the skin gets a leathery structure. The color may become brown-gray. At this stage, the skin is less flexible, which makes working with hands difficult.
The localization varies by type of dermatitis. In case of toxic contact dermatitis, the symptoms mainly occur in areas that come into contact with irritants most: the palms, the fingertips, and between the fingers. In allergic contact dermatitis, the pattern may be more specific, depending on where the contact with the allergen occurs. Nickel allergy, for example, often causes symptoms where jewelry is worn.
In nummular eczema, you see typical coin-shaped, sharply delimited red spots, often on the back of the hand. Atopic dermatitis mainly affects the back of the hand, the wrists and between the fingers, and there are often also complaints on other parts of the body, such as the elbow folds.
Secondary infections can occur when damaged skin becomes contaminated with bacteria. The skin then becomes extra red, warm, swollen and sore. There may be pus coming out of the blisters and you may have a fever. The bacteria Staphylococcus aureus, in particular, is a common cause of skin infections in eczema.
Where does hand eczema appear?
The distribution of hand eczema over the hand often provides an indication of the cause. In case of irritating contact eczema due to frequent hand washing, you usually see the symptoms first on the sides of the fingers and between the fingers. These areas stay wet for the longest time after washing and are therefore the most vulnerable. Later, the symptoms spread to the palms and fingertips. The knuckles can be extra dry and cracked because the skin there is stretched with every movement.
In the case of allergic contact eczema, the pattern may be more specific. An allergy to nickel in rings causes symptoms exactly where the ring is. An allergy to rubber in gloves causes symptoms on the back of the hand and wrists where the glove cuff is located. An allergy to ingredients in hand cream causes symptoms in all areas where you apply the cream.
With atopic eczema, you often see symmetrical symptoms on both hands, especially on the back of the hand, fingertips and wrists. The palms are often spared or less seriously affected. The creases between the fingers may also be affected.
Nummular eczema causes typical coin-shaped patches that can be anywhere on the hand, but often on the back of the hand. These areas are sharply delineated and have a red, scaly edge with a slightly paler central spot.
With a yeast infection, you often see a unilateral infection, usually starting between the fingers, especially between the little finger and ring finger or between the thumb and index finger. The infection can spread to the palm and back of the hand with a typical scaly, slightly raised edge.
Pompholyx or dyshidrotic eczema is a special form in which small, itchy blisters form on the sides of the fingers and on the palms. These blisters are deep in the skin and look like sago grains. They can coalesce into larger vesicles. After a few weeks, the blisters dry up and the skin flakes.
Pompholyx is actually the more severe form with larger blisters or blisters of mild dyshidrotic eczema (also called acrovesicular eczema or vesicular eczema). In practice, however, both terms are often used interchangeably.
Do you suffer from Hand eczema?
Have your skin assessed by a licensed dermatologist via the Skindr app. Upload photos and get a diagnosis with personal advice within 48 hours. No waiting room, no referral required.
Treatment of hand eczema
The treatment of hand eczema consists of various components that are all important. The first and most important thing is to identify and avoid the triggering or irritating factor. Without doing so, any other treatment will only have a temporary effect.
In case of toxic contact eczema
Avoid contact with water, soap and other irritants whenever possible. This is often easier said than done, especially when your work requires it. Wearing protective gloves is then essential. Cotton gloves absorb sweat and protect against mechanical irritation. On top of that, you can wear rubber or latex gloves to protect against water and chemicals.
Do not wash your hands with regular soap but with a soap-free hand rinse or synthetic cleaner. These cleanse without removing the natural fats from the skin. Only wash when really necessary and use lukewarm water. Pat your hands dry and make sure that especially the areas between the fingers are thoroughly dry.
Regular hand greasing is crucial. Use a neutral, oily ointment such as cetomacrogol ointment or petroleum jelly. Oily ointments work better than creams because they last longer on the skin. Apply the ointment several times a day, especially after each hand washing. You can also apply the ointment preventively before you start working.
Before going to bed, you can generously rub your hands with a greasy ointment and then put on cotton gloves for an intensive night treatment.
In case of allergic contact eczema
Identifying and avoiding the allergen is the core of the treatment. Epicutane tests can help determine what you're allergic to. In this test, patches containing various possible allergens are placed on your back. After two days, the doctor assesses whether any reactions have occurred.
Once identified, you should consistently avoid the allergen. This may mean switching to other products, using different work gloves, or even adjusting your work. In case of nickel allergy, you should avoid nickel-containing jewelry and tools. In case of rubber allergy, you should switch to latex-free gloves.
Drug treatment
Cortisone creams suppress the inflammatory response in the skin. Mild preparations are used for children and the elderly, medium strength for adults, and sometimes highly effective preparations for persistent eczema.
It is important to maintain the treatment for a sufficient period of time. Many people stop too early as soon as the symptoms improve, but the inflammation has not completely disappeared by then. This leads to a rapid return of the complaints. Chronic eczema may require maintenance treatment twice a week.
For very pronounced, acute forms, your doctor may prescribe cortisone in tablets. This works systemically and can quickly control a serious outbreak. Tablets are only given for a short time due to possible side effects.
If the eczema is infected (pain, warmth, swelling, and pus), antibiotics are needed as ointments or tablets.
Light therapy
UV therapy can help with persistent chronic hand eczema. Controlled UV irradiation has an anti-inflammatory effect on the skin. The treatment consists of several sessions per week for a few weeks to months.
What doesn't work against hand eczema?
There are various misconceptions about the treatment of hand eczema. Simply lubricating with body lotion or regular hand cream is usually insufficient. These products are too light and often contain perfume that can actually irritate already inflamed skin.
Avoiding cortisone creams for fear of side effects is unjustified. When used correctly on the hands, side effects are rare. The skin on the palms is relatively thick and absorbs less well, so the risk of skin thinning is small. Long-term non-treatment actually leads to chronic eczema, which is much more difficult to treat.
All kinds of alternative ointments and creams with special ingredients such as aloe vera, chamomile or beeswax may sound natural and harmless, but are often ineffective and can actually trigger allergic reactions. In case of acute inflammation, you need proven effective treatment.
The idea that you just have to stop working isn't always realistic or necessary. Adapting your work or way of working, using protective gloves and consistent greasing is often sufficient. However, temporary absenteeism may be necessary in the event of a very serious outbreak.
Trying a diet yourself that omits a variety of foods usually does not help with hand eczema, except in the rare cases where food allergies play a role. Without proper research, you can even cause shortages.
Ignoring a possible yeast infection on the feet is a missed opportunity. If your hand eczema doesn't want to go away despite good treatment, have your feet checked. Treating a foot fungus can sometimes have a miraculous effect on hand eczema.
Frequently asked questions about hand eczema
Is hand eczema contagious?
No, hand eczema is not contagious. You cannot transfer it to others by shaking hands or contact. It is not an infectious disease but an inflammation. If the eczema is infected with bacteria, they can theoretically be transmitted, but in practice this rarely happens and does not necessarily make the other person ill. Of course, good hand hygiene is always important.
Can hand eczema heal completely?
That depends on the cause. Toxic contact eczema can heal completely if you stop contact with the irritant and repair the skin. In case of allergic contact eczema, the allergy usually persists for life, but if you consistently avoid the allergen, the skin stays healthy. Atopic eczema is a chronic predisposition that does not heal, but is easy to treat and manage with the right care.
Can I keep working with hand eczema?
Often yes, but it depends on your work and the severity of the eczema. In some professions such as hairdressers, cleaners or healthcare workers, the risk of hand eczema is high. With the right protection, regular greasing and good treatment, many people can continue to work. Sometimes work adjustment is necessary, or, in serious cases, even a professional change. Discuss this with your doctor and possibly company doctor.
Does hand eczema help improve by going south?
Sunlight does indeed have a beneficial effect on eczema. Many people notice that their hand eczema improves in the summer or while vacationing in sunny areas. The UV radiation has an anti-inflammatory effect. Don't overdo it with sunbathing because burning actually makes the skin more vulnerable. Moderate exposure is best.
Can gloves actually cause hand eczema?
Yes, you can. Rubber or latex gloves can cause sweating, which is irritating. Some people may also be allergic to the rubber chemicals in the gloves. That is why it is important to wear cotton gloves under rubber gloves, change them regularly, and switch to latex-free alternatives in case of allergies. Work gloves that chafe can also cause or worsen eczema.
Should I stop wearing rings?
If you are allergic to nickel, you may need to avoid nickel-containing rings. Moisture and soap can also remain under rings, which can make eczema worse. In the case of active eczema, it is wise not to wear rings temporarily to allow the skin to heal. Then you can wear rings again, preferably made of gold or stainless steel, and take them off regularly to wash and dry the skin underneath.

.webp)