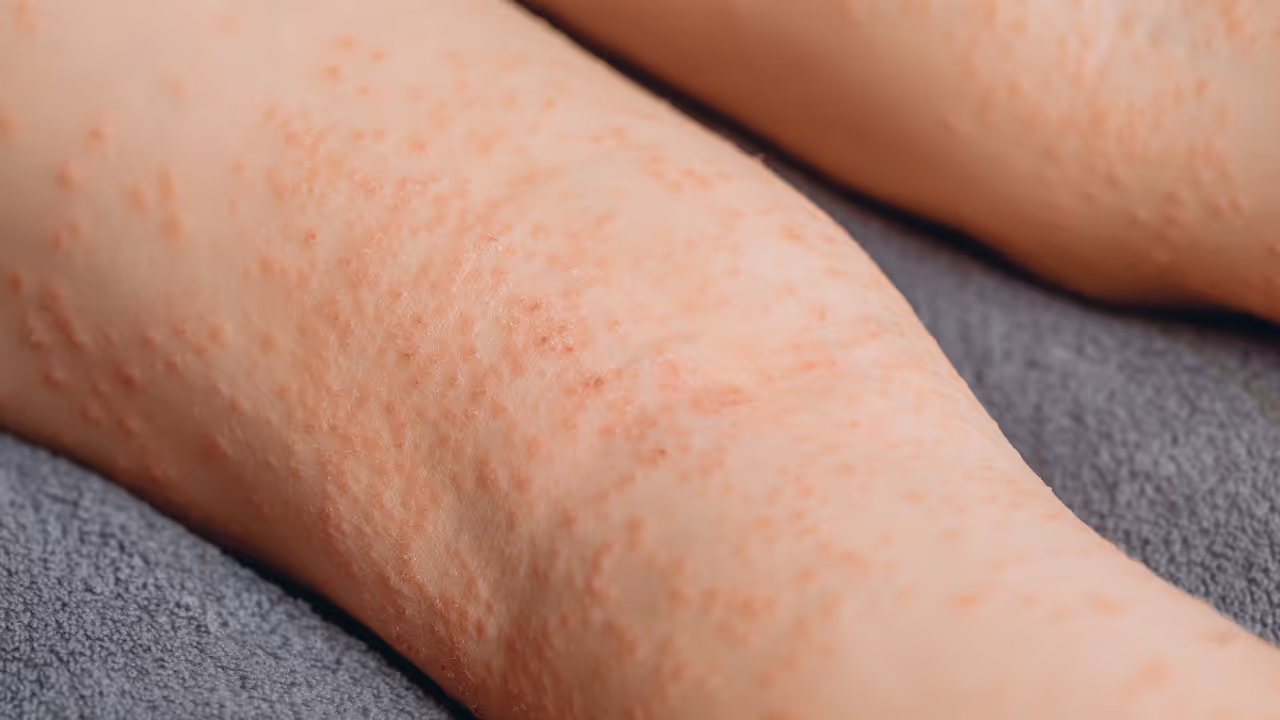
What is a crash on the lower leg?
Rash on the lower leg is a collective name for different types of skin changes that occur between the knee and ankle. These are abnormalities of the normal skin structure, color or texture that can cause discomfort and affect daily life.
Often, the rash looks red and inflamed. This redness occurs because blood vessels in the skin are dilated as a result of inflammatory reactions or blood circulation problems. The redness may be uniform, blemished, or accompanied by brown discoloration with long-term problems. Itching is a common and annoying symptom. The urge to scratch is great, but this further damages the skin and increases the risk of infections.
Scaling often occurs with a rash on the lower legs. The skin is peeling or peeling, which is related to impaired skin cell renewal or dehydration. This gives the skin a dry, rough appearance that worsens especially in the winter. Bumps may be part of the rash. These small imperfections sometimes feel hard, can be painful or, on the contrary, filled with fluid.
Sores or cuts on the lower legs are a more serious sign. These open areas can be damp, are often painful and difficult to heal. They usually indicate blood flow problems or an infection. The rash can be limited to the lower legs, but can also occur on other parts of the body. Sometimes the rash provides indications: bilateral rashes that occur symmetrically on both legs often indicate a systemic problem or skin disorder, while unilateral rash may indicate a local cause or infection.
The location on the lower leg can also provide information. Rashes around the ankles and the bottom of the lower leg are common due to blood flow problems due to varicose veins. Rashes on the front of the tibia may be related to dry skin or specific skin conditions. In the back of the lower leg, in the knee cavity, eczema is more common because this area is more humid and experiences more friction.
Do you suffer from Rash on the lower leg?
Have your skin assessed by a licensed dermatologist via the Skindr app. Upload photos and get a diagnosis with personal advice within 48 hours. No waiting room, no referral required.
How does a lower leg rash occur?
Rashes on the lower leg can occur due to three main categories: circulatory problems, an underlying skin condition, or an infection. Each of these causes has its own developmental pattern and risk factors.
Circulatory problems are a major cause of rash on the lower legs, especially in older people. Varicose veins occur when the valves in the veins of the legs stop working properly. This leads to the accumulation of blood in the legs, especially when standing or sitting for a long time. The increased pressure in the veins allows fluid and proteins to leak through the vascular wall into the surrounding tissue. This causes swelling, brown discoloration and ultimately skin damage.
Varicose eczema, also known as stasis dermatitis, develops gradually. First you see swelling of the ankles and lower legs, especially at the end of the day, and then a brownish discoloration occurs due to iron deposits in the red blood cells. The skin becomes thicker, stiffer and can itch. In advanced stages, open wounds can occur that are difficult to heal, so-called venous ulcers.
Skin disorders on the lower legs can have various causes. Eczema often develops in response to irritants such as soap, wool, or synthetic fabrics in stockings. In people with a genetic predisposition, atopy, the skin barrier is naturally weaker, making the skin more sensitive to stimuli. Crackle eczema occurs due to extreme dehydration of the skin, often in older people in the winter. The skin gets a network of cracks that look like cracked porcelain.
Psoriasis is an autoimmune disorder in which skin cells renew abnormally quickly. The exact cause is unknown, but hereditary predisposition plays a role. Stress, infections, and some medications can trigger or worsen psoriasis. The disorder comes in phases of rest and active periods.
Infections on the lower legs occur when microorganisms enter the skin, often through minor damage. Wound rose, called erysipelas, is caused by streptococcal bacteria that enter through a wound, fungus between the toes, or an insect bite. The infection spreads rapidly through the lymphatic vessels and causes a violent inflammatory response. Cellulite is a deeper infection of the subcutaneous tissue that is more severe and spreads more slowly.
Fungal infections such as ringworm are often transmitted through contact with infected animals, but can also spread from person to person. The fungus grows in the superficial layers of the skin and causes the typical round red spots with a clear border. Warm, humid conditions promote mold growth.
Lyme disease occurs after the bite of a tick that is infected with the Borrelia bacteria. Not all ticks are infected, but when the bacteria is transmitted, the typical red ring forms around the site of the tick bite after a few days to weeks. This rash spreads slowly and is called erythema migrans.
Certain circumstances increase the risk of a rash on the lower legs. Overweight increases pressure on the veins and promotes varicose formation. Standing or sitting for long periods of time before work, such as salespeople or bus drivers, hampers the backflow of blood. Diabetes and cardiovascular diseases increase the risk of circulatory problems and poor wound healing. Age also plays a role: the skin becomes thinner and drier, the blood vessels become less elastic.
Symptoms and characteristics of a lower leg rash
The symptoms of a rash on the lower legs vary greatly depending on the underlying cause. Recognition of specific characteristics helps identify the disorder.
Varicose eczema develops a characteristic pattern with brown discoloration, mainly due to the leakage of red blood cells from the veins. The skin becomes thicker and stiffer, feels warmer and may appear tense due to the accumulation of moisture. Itching is a common symptom that often worsens in the evening. Small red spots or scaly patches may appear. In advanced stages, open wounds can occur that leak fluid and are difficult to heal.
Crackle eczema is characterized by a network of fine cracks in the skin, similar to cracked pottery. The skin is extremely dry, scaly and itchy. It is often painful because the cracks can go deep. The condition worsens in winter due to dry air and heating, and often improves in summer.
Common eczema shows up as red, itchy patches that flake slightly. The boundaries are often not sharp. Crabs can cause spots that secrete moisture. The skin feels rough and may appear cracked. Allergic contact eczema has the same symptoms but occurs after contact with a specific substance.
Psoriasis presents as sharply delineated, red plaques covered with silvery flakes. The plaques feel thickened. The flakes are easily scratched off but red, shiny tissue appears underneath. Psoriasis is usually less itchy than eczema.
Wound dandruff causes sudden, severe symptoms. The skin becomes bright red, warm and shiny, with a sharp border. The red spot spreads rapidly, sometimes within hours. There is severe pain and the skin feels tight. Common symptoms such as fever, chills, and headache are common.
Cellulite has similar but less sharply defined symptoms. The redness is diffuse and spreads more slowly. The skin is swollen, warm and sore when touched. Fever occurs but is often less high than a sore throat.
Ringworm shows distinctive round or oval red spots with a prominent, slightly raised edge and a paler center. The edge may contain small scales. It usually itches moderately and can spread if left untreated.
Erythema migrans in Lyme disease begins as a small red patch that gradually expands into a large, round, or oval red ring, sometimes with a central bright area. The rash is not painful and usually does not itch. Common symptoms such as tiredness and muscle pain may occur.
Erythema nodosum causes painful, raised lumps under the skin. These lumps are 1 to 5 centimetres in size, feel firm, red to purple and very sensitive to touch. After a few weeks, they gradually turn from red to green and yellow, like bruises.
Where does a lower leg rash appear?
Rashes on the lower legs often have specific preferred locations associated with the underlying cause.
Around the ankles and the bottom of the lower leg, the so-called gaiter zone, varicose eczema is most common. This zone experiences the most pressure from accumulating blood in a standing position. The brown discoloration, thickening of the skin and open wounds are concentrated here. Fluid accumulation due to heart failure or kidney disease also first appears around the ankles.
The front of the tibia is a typical location for craquelure eczema because the skin here is naturally drier and there is little subcutaneous fat layer. Psoriasis is also common on the shins, with plaques symmetrically present on both legs. Erythema nodosum, the painful lumps, appear almost exclusively on the front of the lower legs.
The knee and back of the lower leg are sensitive areas for allergic contact eczema and atopic eczema. These areas are more humid due to sweating and experience more friction, which can trigger eczema. In children with atopic eczema, the folds behind the knees are a typical location.
The sides of the lower legs may be affected by extensive skin conditions such as psoriasis or widespread eczema. Fungal infections such as ringworm can occur anywhere on the lower leg, often in several places at the same time.
Wounds and cellulitis can occur anywhere on the lower leg, but often start at an entry point such as a wound, a crack between the toes, or an eczema spot. From there, the infection spreads to the lower leg and can even affect the entire leg if left untreated.
It is important to note that some conditions are not limited to the lower legs. Eczema, psoriasis, and some infections can also occur elsewhere on the body. The presence of a rash on other parts of the body besides the lower legs can actually help make the correct diagnosis.
The distribution over one or both legs also provides information. Bilateral, symmetrical rash often indicates a systemic problem such as varicose eczema, craquelure eczema or psoriasis. Unilateral rash suggests a local cause such as an infection or a specific contact allergen that only acted on one leg.
Do you suffer from Rash on the lower leg?
Have your skin assessed by a licensed dermatologist via the Skindr app. Upload photos and get a diagnosis with personal advice within 48 hours. No waiting room, no referral required.
Treatment of a lower leg rash
Rashes on the lower legs often have specific preferred locations associated with the underlying cause.
Around the ankles and the bottom of the lower leg, the so-called gaiter zone, varicose eczema is most common. This zone experiences the most pressure from accumulating blood in a standing position. The brown discoloration, thickening of the skin and open wounds are concentrated here. Fluid accumulation due to heart failure or kidney disease also first appears around the ankles.
The front of the tibia is a typical location for craquelure eczema because the skin here is naturally drier and there is little subcutaneous fat layer. Psoriasis is also common on the shins, with plaques symmetrically present on both legs. Erythema nodosum, the painful lumps, appear almost exclusively on the front of the lower legs.
The knee and back of the lower leg are sensitive areas for allergic contact eczema and atopic eczema. These areas are more humid due to sweating and experience more friction, which can trigger eczema. In children with atopic eczema, the folds behind the knees are a typical location.
The sides of the lower legs may be affected by extensive skin conditions such as psoriasis or widespread eczema. Fungal infections such as ringworm can occur anywhere on the lower leg, often in several places at the same time.
Wounds and cellulitis can occur anywhere on the lower leg, but often start at an entry point such as a wound, a crack between the toes, or an eczema spot. From there, the infection spreads to the lower leg and can even affect the entire leg if left untreated.
It is important to note that some conditions are not limited to the lower legs. Eczema, psoriasis, and some infections can also occur elsewhere on the body. The presence of a rash on other parts of the body besides the lower legs can actually help make the correct diagnosis.
The distribution over one or both legs also provides information. Bilateral, symmetrical rash often indicates a systemic problem such as varicose eczema, craquelure eczema or psoriasis. Unilateral rash suggests a local cause such as an infection or a specific contact allergen that only acted on one leg.
What doesn't work against a lower leg rash?
There are many misconceptions about treating rashes on the lower legs that are not only ineffective, but sometimes even worsen the situation.
The idea that scratching provides relief and does no harm is wrong. Scratching damages the skin barrier, increases the risk of infections and worsens the inflammatory response. Especially with varicose eczema, where the skin is already vulnerable, scratches can lead to open wounds that are very difficult to heal. Cut your nails short and try to find distracting activities when itching hits.
Waiting too long to treat varicose eczema in the hope that it will go away on its own leads to progressive skin damage. The longer the skin changes exist, the harder they are to treat. Open wounds can occur that last for months to years. Early treatment with compression therapy can prevent much suffering.
Self-medication with all possible creams and ointments at the same time makes it difficult to determine what works. In the event of a problem, you will not see that the treatment itself can cause irritation. Introduce new products one by one.
Using hot water and harsh soap to relieve itching is counterproductive. This further dries out the skin and worsens eczema and craquelure eczema. Use lukewarm water and mild cleansers. A wash oil is often better than soap for dry skin.
Wearing compression stockings without medical advice and without the right size and strength can be ineffective or even harmful. Too tight compression can actually restrict blood circulation. Too weak compression does not provide sufficient support. If necessary, have compression socks fitted by a bandagist.
Ignoring signs of an infection such as dandruff or cellulitis is dangerous. These infections can spread rapidly and lead to serious complications such as septicemia. Sudden increases in redness, swelling and pain, combined with fever, requires immediate medical attention.
The idea that you should always wait for the results to go away on their own is unwise. Some conditions are chronic and require ongoing treatment. Early intervention prevents complications and long-term inflammation.
Frequently asked questions about lower leg rash
Is a rash on the lower leg contagious?
This depends on the cause. Infections such as dandruff and yeast infections can be contagious. Fungal infections can be transmitted through direct contact or shared towels and shoes. Skin conditions such as eczema, psoriasis, and varicose eczema are not contagious. You can't contract them through contact with someone who has these conditions, although hereditary predisposition may play a role.
How long does a rash on the lower leg last?
The duration varies greatly. Acute rash due to irritation often disappears within a few weeks. Varicose eczema and psoriasis are chronic conditions that can last for years and require permanent treatment. Crackle eczema usually improves in the summer but returns in the winter. Infections such as dandruff heal with antibiotics within one to two weeks. Fungal infections require at least two weeks of treatment. Erythema nodosum disappears spontaneously within four to six weeks.
Does laying the leg high help?
Yes, with varicose eczema and fluid retention, laying a leg high helps considerably. Raise your legs higher than your heart for 15 to 30 minutes several times a day. This promotes venous return and reduces swelling. At night, you can raise the foot of your bed a few inches. In the case of infections such as dandruff, rest and high also helps with recovery. In other skin conditions, laying high has no direct effect on the rash itself.
When should I see a doctor?
Consult a doctor in case of sudden, painful redness with fever, which may indicate dandruff or cellulitis. Even with a rash that does not improve after two weeks of self-treatment, with open wounds that do not heal, with severe itching that disrupts your sleep, or with increasing swelling and pain. If you have diabetes and develop a rash or sores on your lower legs, medical assessment is extra important because of the increased risk of complications.
Can varicose veins disappear again?
Existing varicose veins do not disappear spontaneously. Compression therapy may reduce symptoms of varicose eczema but does not repair damaged valves in the veins. There are treatments to remove or close varicose veins, such as sclerotherapy where the vein is closed or surgical removal. These treatments can be considered for serious complaints or cosmetic concerns.
Is a rash on the lower leg dangerous?
Usually not immediately dangerous, but some causes require urgent attention. Wound dandruff and cellulitis can spread rapidly and cause septicemia if left untreated. Open wounds in varicose eczema can become chronic and difficult to heal, which significantly affects the quality of life. Erythema nodosum may indicate an underlying systemic disease that requires treatment. Early medical assessment helps prevent serious complications.

.webp)