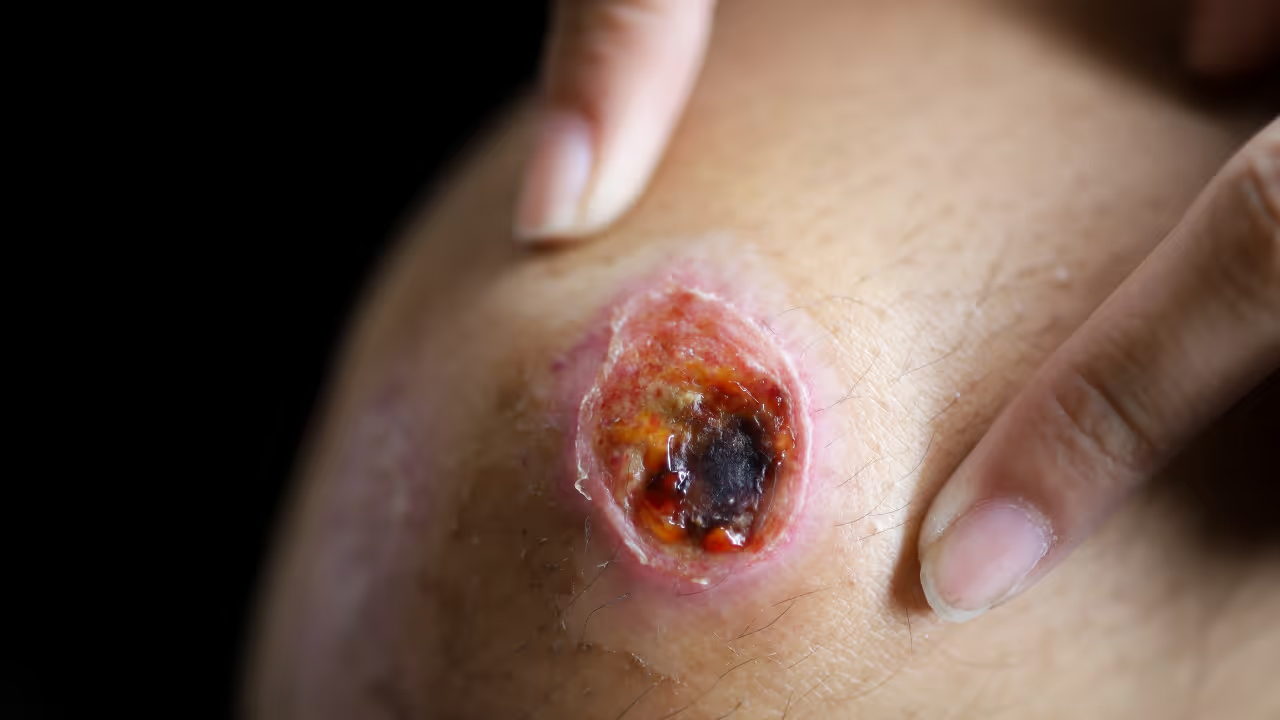
What is an open wound on the leg?
An open wound on the leg, medically called ulcus cruris, is skin damage that has lost the entire skin tissue including the deeper layers. The characteristic problem with these wounds is that they heal poorly or not at all, even after weeks or months. This distinguishes them from ordinary wounds that usually close within a few weeks.
The underlying causes are diverse but are often related to impaired healing due to blood circulation problems. Poor circulation means that insufficient oxygen and nutrients reach the wound, and that waste products are not properly removed. This inhibits the natural healing process.
Varicose veins are a common cause. In the case of varicose veins, the valves in the leg veins no longer work properly, causing blood to stagnate in the legs. This leads to increased pressure in the veins, fluid accumulation in the tissue, and ultimately to skin damage. Wounds caused by varicose veins are called venous ulcers and are the most common.
Arteriosclerosis can also lead to open wounds. In arteriosclerosis, the arteries are narrowed, so that too little blood flows to the legs. Tissues then receive insufficient oxygen, which can lead to wounds that do not heal. These arterial ulcers often feel different from venous wounds and are located in different areas.
Diabetes is an increasingly important cause. Long-term diabetes can damage both blood vessels and nerves. The reduced sensitivity in the feet means that minor injuries go unnoticed, while poorer blood circulation and increased blood sugar make healing difficult. Diabetic foot ulcers require special attention because they can lead to serious complications.
In bedridden people, pressure sores can occur from lying in the same place for a long time. These bedsores or pressure sores can also develop into deep open wounds if they are not treated in time. The constant pressure on certain parts of the body disrupts blood flow to the skin, causing tissue to die.
Open leg wounds have a major impact on your daily life. They can be painful, cause an unpleasant odor, and restrict your mobility. The risk of infections has also increased. The treatment often requires a lot of patience and a combination of different measures.
Do you suffer from Open leg wound?
Have your skin assessed by a licensed dermatologist via the Skindr app. Upload photos and get a diagnosis with personal advice within 48 hours. No waiting room, no referral required.
How does an open wound on the leg develop?
The development of an open leg is usually a gradual process in which several factors play together. Venous problems caused by varicose veins often start with heavy, tired legs at the end of the day. The veins can become visible as blue-green serpentine lines under the skin. Due to increased pressure in the veins, fluid from the blood vessels begins to leak into the surrounding tissue, leading to swollen ankles and lower legs.
This accumulation of fluid, called edema, eventually disrupts the skin's nutrition. The skin becomes thinner and more vulnerable. You often see a brownish discoloration of the skin around the ankle. This is caused by blood pigment that leaks from the veins and builds up in the skin. The skin can also feel harder and stiffer, known as lipodermatosclerosis.
A minor injury, for example due to bumps, scratches or even just because of the shoe, can then be the trigger for an open wound to occur. With healthy skin, such a small wound would heal within a few days, but with damaged skin with poor circulation, this will not work. The wound remains open and may even grow larger. The moisture that comes out of the wound can further damage the surrounding skin, causing the wound to spread.
In the case of arterial problems, the process is different. Due to the narrowing of the arteries, the legs receive too little oxygen-rich blood. You often notice this first while walking, when the muscles need more oxygen. You get calf pain that disappears when you stand for a while, which is called claudication or leg pain. Later, pain can also occur at rest, especially in bed at night. The skin becomes pale and cool to the touch. Small wounds do not heal because there is simply too little blood.
In diabetes, nerve damage plays an additional role. Because of the damaged nerves, you don't feel as well as what you're standing on and you don't notice minor injuries in time. Elevated blood sugar levels also provide a favorable environment for bacteria, making wounds easy to infect. The combination of reduced sensitivity, poorer blood flow and increased susceptibility to infection makes diabetic wounds particularly difficult.
Pressure sores in bedridden patients occur because the body weight constantly presses on certain points such as the heel, rump or elbows. This constant pressure compresses the small blood vessels, so that the tissue no longer receives oxygen. Initially, you only see a redness that does not disappear when you press on the skin. If the pressure is not relieved, the tissue dies and an open wound occurs that can quickly deepen.
Symptoms and characteristics of an open leg wound
An open leg is recognisable as a wound where the entire thickness of the skin has been lost. This means that not only the superficial layer of the skin, but also the deeper layers, including the hair roots, are damaged. You are literally looking into the underlying tissue. This distinguishes an ulcer from superficial abrasions that only touch the top layer of the skin.
The wound is usually on the inside of the ankle, just above the ankle bones. This is a typical site for venous ulcers because this is where the pressure in the veins is highest. Arterial ulcers are more commonly found on the toes, the foot, or on the outside of the lower leg where blood flow is the least. Diabetic ulcers are mainly found underfoot in areas that get a lot of pressure while walking.
The color of the wound provides information about the condition. A red or pink-red color with shiny tissue is a good sign and indicates healthy granulation tissue that is healing. A yellow color indicates the presence of fibrin and dead tissue that must be removed to allow healing. A black color means that there is necrotic, i.e. dead, tissue. This dead tissue must be removed because it blocks healing and can serve as a breeding ground for bacteria.
The edge of the wound is also important. In the case of a venous ulcer, the edge is often flat and irregular. In the case of an arterial ulcer, the edge may actually be sharply defined. A hardened, swollen edge may indicate an inflamed wound. Undercut edges where the wound under the skin extends further than you see on the surface occur in certain infections and pressure sores.
The area around the wound also tells a story. In case of venous problems, you often see a brown discoloration of the skin around the wound, swollen ankles, and sometimes varicose veins. The skin can feel stiff and hard. In case of arterial problems, the skin is pale, cool and smooth. There is little hair left and the toenails grow slowly and become thick. In diabetes, there may be several small wounds, and the foot may have an abnormal shape due to nerve damage.
Pain is a variable symptom. Venous ulcers are often surprisingly unpainful, although they can feel uncomfortable. Arterial ulcers, on the other hand, are often very painful, especially at rest and at night. In diabetic ulcers, you often feel no pain at all due to nerve damage, which is dangerous because it is easy to overlook the wound.
Moisture can leak out of the wound, which is called exudate. The amount and color of these varies. Clear or light yellow fluid is normal for a healing wound. Cloudy, greenish or foul-smelling moisture indicates an infection. A lot of moisture production can damage the surrounding skin and make the wound larger.
Where do open wounds on the leg occur?
The location of an open leg is strongly related to the underlying cause. Venous ulcers, the most common form, are almost always on the inside of the ankle. This region is called the medial malleolar region. Sometimes you see wounds on both ankles symmetrically. The preferred location has to do with the anatomy of the veins and the highest venous pressure at this location. Venous wounds can become quite large and often have irregular edges.
Arterial ulcers have a different distribution. They are often located in areas that are farthest from the heart and where blood flow is the least. Think of the toes, the top of the foot, the heel, or the outside of the lower leg. These wounds are usually smaller and deeper than venous ulcers, with sharply defined edges. They can be very painful because the tissue lacks oxygen.
In diabetic foot ulcers, the focus is on the sole of the foot. Pressure points under the big toe, the ball of the foot, or the heel are typical areas. These areas receive the most load when walking. Due to the reduced sensitivity, the patient does not notice that there is too much pressure on these points, and damage occurs. Sometimes you also see wounds between the toes where fungal infections can play a role, or where the shoe rubs.
Mixed ulcers, involving both venous and arterial problems, can occur anywhere on the lower leg. The combination of both problems makes the treatment extra challenging because some measures that help with venous problems can actually be harmful to arterial problems.
Pressure sores in bedridden patients occur at pressure points. On the legs, these are mainly the heels, the ankle bones on the outside and inside, and the knees when someone often lies on their side. These wounds can get deep quickly because the body weight pressure is very high on a small surface.
Do you suffer from Open leg wound?
Have your skin assessed by a licensed dermatologist via the Skindr app. Upload photos and get a diagnosis with personal advice within 48 hours. No waiting room, no referral required.
Treatment of an open wound on the leg
The treatment of an open leg consists of several parts that are all important. The first and most important thing is to address the underlying cause. Without doing this, the wound will barely heal, no matter what local treatment you use.
In venous ulcers, compression therapy is the cornerstone of treatment. This means wearing elastic bandages or compression socks that put pressure on the leg. This pressure helps to squeeze fluid out of the leg and improves the functioning of the veins. Elastic bandages are applied from the foot up, with the strongest pressure at the ankle gradually decreasing towards the knee. You wear these bandages day and night and only remove them for daily body care and wound care. It is important to apply the bandage in the morning when the leg is still relatively slim.
Compression socks are an alternative to bandages, especially for maintenance and prevention. These stockings are custom-made and there are different strength classes. For venous problems, class 2 is usually used. Putting on these stockings can be difficult, but there are tools that make this easier. In special cases, pneumatic compression can be used, putting an inflatable boot around the leg that swells and deflates rhythmically to squeeze moisture out of the leg.
In the case of arterial problems, compression is dangerous because it would further obstruct the already limited blood supply. Here, the focus is on restoring blood flow. This can be done by medication that dilates the blood vessels, but sometimes surgery is necessary to widen or bridge narrowed arteries. Quitting smoking is crucial because smoking further constricts the blood vessels.
In the case of diabetes, blood sugar levels must be controlled as well as possible. High sugar levels inhibit healing and increase the risk of infection. Pressure relief is also essential for diabetic foot ulcers. This means special shoes, insoles or even temporarily not walking on the affected foot at all. Regular monitoring by a specialist diabetic foot team is important.
Local wound treatment focuses on creating optimal conditions for healing. Dead tissue and scabs must be removed because they block healing. This can be done mechanically by cleaning the wound and gently loosening the batter in a bath. Stubborn dead tissue may require surgical debridement, where the dead tissue is excised under local anaesthesia.
The wound should be kept moist but not too wet. Modern wound dressings help with this. There are different types depending on the amount of moisture that the wound produces. Absorbent bandages are used when there is a lot of moisture, but moisturizing bandages are used for dry wounds. The bandage should be changed regularly, but not too often because every bandage change can also damage healthy tissue.
Antibiotics are needed in case of infections. SuperFICIAL infection is sometimes treated with local antiseptic agents, but a real deep infection requires oral antibiotics or even intravenously. Signs of infection include increasing pain, redness and swelling around the wound, pus, an unpleasant odor, and fever.
Underlying conditions must be treated. Anemia can inhibit healing and needs to be corrected. Heart failure can cause fluid buildup in the legs and requires treatment. Malnutrition, especially protein deficiency, inhibits wound healing and requires dietary adjustment.
If conservative measures do not work, plastic surgery may be considered. In this procedure, the wound is cut into the healthy tissue and covered with a skin graft. This is a piece of thin skin taken from another spot, usually the upper thigh, and stitched onto the wound. In around eighty percent of the cases, this procedure is successful. The condition is that the underlying cause has been addressed, otherwise the wound will recur.
After the wound has healed, good aftercare is essential to prevent the wound from coming back. In case of venous problems, this means wearing compression stockings for life. In case of arterial problems, taking medication and quitting smoking. In diabetes, strict blood sugar control and daily inspection of the feet.
What doesn't work against an open leg wound?
There are several misconceptions about the treatment of open legs. Just cleaning and putting a bandage on it is not enough. Without addressing the underlying cause, the wound will not heal or recur again and again. This is frustrating for patients who sometimes faithfully care for their wounds for months without improvement.
In the case of venous ulcers, resting is counterproductive. People sometimes think that with a leg wound, you should mainly rest and raise the leg. Although raising your leg does indeed help reduce fluid, too much rest is actually bad. Exercise activates the pumping function of the calf muscles, which helps to force blood from the legs back to the heart. Walking with compression socks on is one of the best things you can do.
Removing scabs or dead tissue yourself without expert guidance can be dangerous. You can damage healthy tissue, cause bleeding, or push bacteria deeper into the wound. Debriding wounds is a profession that requires expertise.
All kinds of home remedies such as honey, coffee grounds, vegetable oils or pharmacy ointments generally do not help with chronic leg injuries. These medicines can sometimes even be harmful by triggering allergic reactions or promoting bacterial growth. Modern wound dressings have been specifically developed to create optimal conditions for healing.
With arterial ulcers, compression therapy is dangerous. If there is insufficient blood supply, applying tight bandages can further hamper the flow and aggravate the situation. This can even lead to tissue death. That is why it is important to always measure the ankle brachial index before starting compression therapy, a simple exam that measures the ratio between the blood pressure in the ankle and the arm.
Ignoring pain or other alarm signals is dangerous. Increasing pain, fever, or sudden worsening of the wound may indicate a serious infection that requires acute treatment. Especially among diabetics, infections can escalate rapidly and lead to life-threatening situations.
Frequently asked questions about open wounds on the leg
How long does it take for an open leg to heal?
This varies greatly depending on the size of the wound, the underlying cause, and how well the treatment is followed up. Small venous ulcers can heal in six to twelve weeks with good compression therapy. Larger wounds can take months to even a year. Arterial ulcers usually heal more slowly and only if blood flow can be restored sufficiently. Diabetic foot ulcers also often require months of treatment. Patience is essential.
Can an open leg come back after healing?
Yes, unfortunately, the chance of recurrence is quite high, especially with venous ulcers. Around half of the healed venous ulcers will return within a few years if you don't keep wearing compression socks consistently. In case of arterial problems, it depends on the severity of the vasoconstriction. In diabetes, good blood sugar control and daily foot inspection are essential to prevent new wounds. Prevention requires lifelong attention.
Can you shower or bathe with an open leg?
Showering is certainly allowed and is even important for hygiene. Let the water flow past the wound but do not spray directly onto the wound. Bathing is also possible, although some doctors do not recommend this for infected wounds. Then dry the leg thoroughly and apply a new bandage. Don't wash too often, once a day is usually sufficient. Do not use soap directly on the wound, but do apply it to the surrounding skin.
Is an open leg wound contagious?
No, an open leg itself is not contagious. It is not an infectious disease that you can pass on to others. However, the wound can become infected with bacteria, but that infection is also not contagious in the sense that it does not make others ill. Of course, good hygiene is important, especially if you care for the wound yourself. Wash your hands before and after taking care of the wound.
When is surgery necessary?
Surgery is considered if the wound does not heal despite months of conservative treatment, if the wound is actually getting bigger, or if a malignant change in the wound is suspected. In case of arterial problems, surgery may also be necessary to restore blood flow. In the case of extensive varicose veins, surgery to remove them can help heal the wound and prevent new wounds.
Can I keep working with an open leg?
That depends on your work and the severity of the wound. Work that involves a lot of standing is generally not recommended because it worsens the accumulation of fluid. Seated work or work where you can alternate between sitting, standing and walking is often possible. Discuss with your doctor and possibly company doctor what is wise in your situation. Wearing compression socks while working is usually possible and even necessary.

.webp)