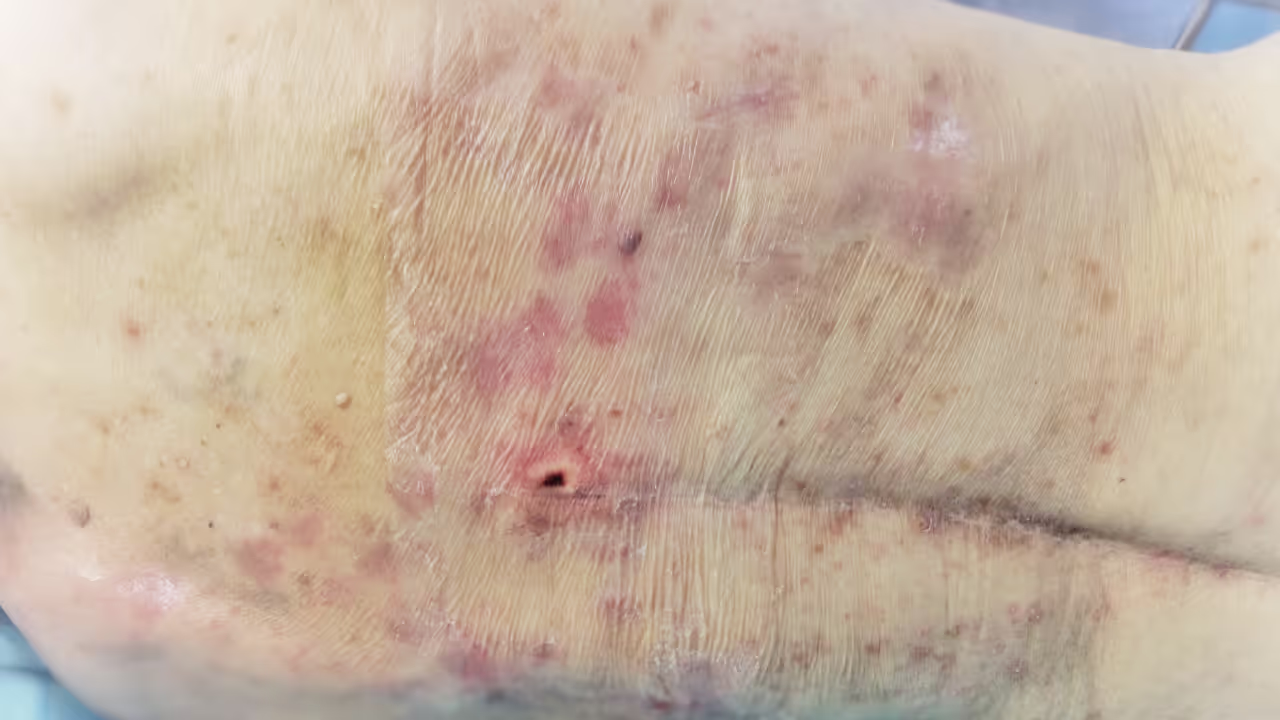
What are pressure sores?
Bedsores, called pressure sores in medical terms, are skin lesions that occur when pressure or friction is applied to the same area for too long. Your skin needs oxygen and nutrients that are supplied via the blood. If there is prolonged pressure on a certain area, the blood vessels are compressed and the tissue does not receive enough oxygen. This leads to damage to the skin and underlying tissue.
The condition mainly occurs in places where there is little tissue between the bone and the skin. Think of the heels, the rump at the bottom of the back, and the side of the hips. At these pressure points, the skin can be damaged more quickly because there is little protection between the bone and the outside world.
Bedsores develop gradually at different stages. At first, all you see is a red spot that doesn't disappear when you press it. This is an important warning sign that the skin is under pressure. If the pressure is not removed, the damage can go deeper and eventually an open wound occurs. In severe cases, even muscles, tendons and bones can become visible.
The disorder mainly affects people who have to stay in one position for a long time, such as bedridden patients or people in wheelchairs. Older people are also at increased risk, because their skin is often thinner and more vulnerable. People with nerve damage have an extra risk because they often do not feel when there is too much pressure on the skin, so that the warning sign of pain is missing.
Do you suffer from Bedsores?
Have your skin assessed by a licensed dermatologist via the Skindr app. Upload photos and get a diagnosis with personal advice within 48 hours. No waiting room, no referral required.
How do pressure cores develop?
The development of bedsores begins with impaired blood circulation due to prolonged pressure. When you lie or sit in the same position for a long time, the blood vessels between the bone and the surface of the skin are compressed. The skin cells then receive insufficient oxygen and nutrients, and waste cannot be removed properly. This leads to damage and ultimately to tissue death.
Friction and shear forces worsen the situation considerably. When someone in bed is pulled up or down instead of being lifted, the different layers of skin slide over each other. This damages blood vessels and tissue even faster than pressure alone. Medical equipment such as bladder tubes or oxygen tubes can also cause pressure sores when the patient lies on them or if the material is too tight.
Various factors make people extra sensitive to developing bedsores. Decreased immunity weakens the skin's natural repair mechanisms. This often occurs in people with serious illnesses, after surgeries, or chemotherapy. Malnutrition also plays an important role, because without sufficient protein, vitamins and calories, the skin cannot recover properly.
Moisture has an undermining effect on the skin. People with incontinence are at extra risk because urine and faeces contain irritants that affect the skin. Moisture also makes the skin softer and more vulnerable, causing it to be damaged more quickly. Excessive sweating can also weaken the skin and increase the risk of bedsores.
Nerve damage is a particular risk because the body's natural warning system fails. Normally, you feel discomfort or pain when you sit or lie in the same position for too long, so you will automatically change your position. People with nerve damage due to diabetes, spinal cord injury or other neurological disorders, for example, miss this signal and stay in the same position for too long.
Symptoms and characteristics of pressure sores
Bedsores develop in four categories that are becoming increasingly severe. Recognizing the early signs is crucial to prevent further damage. Bedsores often develop rapidly, and without intervention, an incipient red spot can grow into a serious wound within days.
In category 1, you see a red spot on the skin that does not disappear when you press it. This is the first and most important warning sign. The skin is still intact, but the tissue underneath has already been damaged by the pressure. The area may also feel warm, hard, or swollen. In people with dark skin, this redness is more difficult to see, so bedsores are often only discovered at a later stage.
Category 2 is characterized by superficial skin damage. The skin is red and there has been visible damage, such as a blister or a superficial abrasion. It looks like an abrasion or burn blister. The area is sensitive and can hurt when touched. If the pressure is not removed now, the damage will quickly deepen.
In category 3, the skin is more deeply damaged and an open ulcer occurs. You can see the fat layer under the skin, but no muscles or bones yet. The wound may contain fluid or pus and the edges are often raised or swollen. At this stage, professional medical care is absolutely necessary because the risk of infection is high.
Category 4 is the most serious form where the damage goes so deep that tendons, muscles or even bone become visible. The wound is deep and may contain black or dead tissue debris. There is often a high risk of infections that can spread to the bone or bloodstream, which can be life-threatening.
Where do pressure sores occur?
Bedsores always occur in areas where bones lie close to the surface of the skin and where prolonged pressure is exerted. The location is strongly related to the position in which someone spends most of their time and with any medical material that exerts pressure.
In people who lie mainly on their backs, bedsores often occur on the back of the head, shoulder blades, elbows and especially the coccyx. The heels are particularly sensitive and this is where the first signs of bedsores often occur. The spine can also be affected, especially if the head of the bed is raised too much and the patient slides down.
People who lie on their sides a lot are more likely to get bedsores on the side of the head, shoulders, hips, side of the knees, and ankles. The hip is a particularly vulnerable spot when lying sideways because a lot of weight rests on a small surface here. Therefore, when lying sideways, it is important not to lie completely on the side, but slightly tilted on the back.
For people in wheelchairs, the seats are the most risky places. The buttocks and rump carry the full body weight and are under pressure for hours. The back of the thighs and the shoulder blades can also cause problems, especially when someone sinks into the chair. The feet are at risk if they are not properly supported or if they press against the wheelchair's footplates.
Medical equipment is an often underestimated source of pressure sores. Bladder probes, infusion tubes, oxygen tubes, and respirators can all create pressure points in unexpected places. A cuff that is too tight for measuring blood pressure, elastic stockings or support stockings can also cause damage if worn for a long time. Even a crease in the sheet can lead to problems with very sensitive skin.
Do you suffer from Bedsores?
Have your skin assessed by a licensed dermatologist via the Skindr app. Upload photos and get a diagnosis with personal advice within 48 hours. No waiting room, no referral required.
Treatment of pressure sores
The treatment of bedsores requires a coordinated approach where different healthcare providers work together. Prevention always comes first, because preventing a bedsore is much more effective than curing. As soon as a bedsore occurs, acting quickly is essential to limit further damage.
The most important thing in treatment is to remove the pressure on the affected area. This means changing positions regularly, ideally every two to four hours, depending on the vulnerability of the skin. When moving, it is crucial to lift the patient instead of pushing or pulling, as shear forces further damage the tissue. Aids such as a glide or hoist can help with this.
Special mattresses and pillows play an important role in the treatment. There are different types that distribute pressure better across the body. Some mattresses contain air that circulates or whose pressure changes continuously, so that no point is pressurized for a long time. Water mattresses and gel pillows can also help. The choice depends on the severity of the bedsore, the patient's mobility and practical considerations such as the ability to disinfect the mattress properly.
Wound care is essential for existing bedsores. The wound should be cleaned regularly and bandaged with appropriate materials that create a moist wound environment, which promotes healing. Dead tissue must be removed because it can cause infections and prevent healing. This is done by a specialist nurse or doctor. In case of signs of infection such as increasing redness, swelling, warmth, pus or fever, antibiotics are needed.
Nutrition plays a crucial role in the healing process. The skin needs protein, vitamins, and minerals to recover. A dietician can advise on the optimal composition of the diet and can prescribe extra protein-rich supplements. Sufficient fluid intake is also important for good blood circulation and wound healing.
Severe bedsores of category 3 and 4 may require surgical treatment. Dead tissue must then be surgically removed. In some cases, a skin transplant or moving healthy tissue to the wound is considered, but this is only possible if the patient's general health allows it and if the underlying causes have been addressed.
What doesn't work against pressure sores?
There are many misunderstandings about the treatment and prevention of bedsores. Massaging the skin at pressure points is often done with the best intentions, but does not work and can even be harmful. Massaging actually further damages the delicate blood vessels in the tissue under the skin, especially in places where bones lie close to the surface. Instead of massaging, it is better to gently lubricate the skin with protective cream without rubbing.
Blankets and sheets with pleats seem harmless, but can already cause problems for fragile skin. Smearing out creases does help to avoid unnecessary pressure points. The use of traditional diaper bags or nappies that do not absorb moisture properly also increases the risk of bedsores due to constant humidity.
Staying in the same position for too long because someone seems to be asleep or because you don't want to disturb them is a common mistake. Changing positions regularly remains necessary, even at night. Awakening the patient is a smaller price than the development of a bedsore that can last for months.
Thinking that only bedridden patients are at risk is a dangerous misconception. People who sit in a chair for a large part of the day are also at risk. This not only applies to wheelchair users, but also to people who spend a lot of time in an armchair due to illness or old age. They, too, need to change their posture regularly and relieve pressure points.
Ignoring early warning signs such as a red spot that doesn't go away always leads to worsening. You can often completely prevent a bedsore in category 1 by taking the pressure off immediately. Waiting for it to go away on its own almost always results in further damage. Early intervention is the key to success.
Frequently asked questions about pressure problems
How long does it take for a bedsore to occur?
A bedsore can begin to occur within a few hours in people with very fragile skin and reduced blood flow. It takes longer for healthy people, but they can also develop red spots after a day of lying in the same position. The rate depends on the amount of pressure, the fragility of the skin, the nutritional condition and the presence of moisture.
Can bedsores heal completely?
Bedsores in categories 1 and 2 usually heal completely without scars if the pressure is removed and the wound is properly cared for. Deeper bedsores of categories 3 and 4 heal more slowly and often leave scars. The healing process can take weeks to months, and the skin in that area remains more vulnerable to new bedsores.
Are bedsores contagious?
No, bedsores are not contagious. You can't contract them through contact with someone who has a bedsore. However, bacteria in an infected bedsore can be transferred to other wounds, which is why good hand hygiene is important when caring for wounds.
Can anyone get bedsores?
In theory, anyone can get bedsores if enough pressure is applied to the same area for long enough. In practice, however, they mainly occur in people with reduced mobility, elderly people, people with malnutrition, and disorders that affect blood flow or sensation. Healthy, active people who change positions regularly are at virtually no risk.
How do you prevent bedsores in someone who is being cared for at home?
Prevention at home is about changing positions regularly, a good mattress or seat cushion, attention to nutrition and sufficient moisture, good skin care, and treating incontinence quickly. Check the skin daily for pressure points, especially the heels, rump and hips. Involve the doctor and district nurse in care and follow their advice.
Are there tools that help with prevention?
Yes, there are various tools. Anti-decubitus mattresses distribute pressure better over the body. Special seat cushions help people who sit a lot. Heel cushions can relieve the heels. Sliding sails help to move people without shear forces. Many of these aids are available through home care stores and are sometimes reimbursed by the health insurance fund.
When should you contact the doctor?
Contact us at the first signs of a bedsore, i.e. remove a red spot that does not disappear after pressure. Even if an existing bedsore worsens, signs of infection such as fever, increasing pain, pus or an unpleasant odor, or if the bedsore does not heal despite good care, you should consult your doctor immediately.
Resources
- Gezondheidenwetenschap.be: Preventing bedsores
- Federal Health Care Knowledge Center (KCE): A national guideline for pressure ulcer prevention, 2013
- V&VN Knowledge Institute: Postures and aids for bedsores
- Wit-Gele Kruis: Aids for and against bedsores
- www.ebpnet.be

.webp)